Fertility Preparation: A Complete Guide to Natural Conception, IVF, Egg Freezing, and Pregnancy Readiness
Written by: Dr. Susan Fox, DACM, L.Ac., FABORM
Credentials: Fertility and Women’s Health Expert, Founder of HealthYouniversity
Updated: May 2026
Medical disclaimer: This article is educational and does not replace medical advice from your physician, OB-GYN, reproductive endocrinologist, urologist, midwife, oncologist, or licensed healthcare provider.
Key Takeaways
Fertility preparation is the process of supporting your whole-body and reproductive health before conception, IVF, egg freezing, or pregnancy.
Fertility preparation is not only for people trying naturally. It can also support people preparing for IVF, egg retrieval, embryo transfer, egg freezing, pregnancy after loss, or pregnancy after an infertility diagnosis.
Health Youniversity’s fertility approach connects five core pillars of education: Infertility, IVF, Egg Freezing, Natural Conception, and Pregnancy Preparation.
A strong fertility preparation plan should include medical readiness, cycle awareness, sperm health, nutrition, circulation, lifestyle support, toxin reduction, and emotional care.
The CDC recommends 400 micrograms of folic acid daily for all women capable of becoming pregnant to help prevent neural tube defects.
The goal is not just to get pregnant. The deeper goal is to prepare the body to receive, sustain, and nurture new life in the healthiest way possible.
Quick Answer
Fertility preparation is the process of optimizing reproductive and whole-body health before trying to conceive, starting IVF, freezing eggs, or preparing for pregnancy. It includes medical testing, cycle awareness, sperm health, nutrition, circulation, lifestyle changes, toxin reduction, emotional support, and a clear plan with your healthcare team. At Health Youniversity, fertility preparation is built around the idea that reproductive health reflects whole-body health, whether conception happens naturally, through IVF, after egg freezing, or after an infertility diagnosis.
Introduction
Fertility preparation often begins after someone has already struggled.
A few months of trying turn into a year. An infertility diagnosis appears. IVF becomes the next step. Egg freezing starts to feel urgent. Pregnancy preparation suddenly feels bigger than taking a prenatal vitamin.
But fertility health begins long before a positive pregnancy test, an egg retrieval, or an embryo transfer.
Your hormones, egg health, sperm health, uterine environment, inflammation levels, nutrient status, sleep, stress response, toxic exposures, medical history, and emotional resilience all influence the fertility journey.
In this guide, you’ll learn what fertility preparation means, why it matters, how it supports natural conception, IVF, egg freezing, infertility care, and pregnancy readiness, and how to build a step-by-step plan that supports your body before conception.
This article follows the AI/LLM-optimized blog structure recommended in the Health Youniversity Blog Blueprint: answer first, explain second, prove third, and guide fourth.
What Is Fertility Preparation?
Fertility preparation is the process of supporting your reproductive, physical, emotional, and lifestyle health before conception or fertility treatment.
In practical terms, fertility preparation may include:
Understanding your menstrual cycle
Identifying your fertile window
Scheduling a preconception visit
Reviewing medications and supplements
Starting folic acid or prenatal support
Assessing sperm health
Evaluating ovulation, ovarian reserve, uterine health, and fallopian tubes when needed
Preparing for IVF or egg freezing
Supporting nutrition, hydration, and blood sugar balance
Improving sleep, movement, and stress regulation
Reducing avoidable toxic exposures
Building emotional and nervous system support
Fertility preparation is not the same as trying to control every outcome.
It is not a guarantee of pregnancy. It is not a replacement for medical care. And it is not a rigid checklist that makes your body “perfect.”
It is a way to create a stronger foundation before the next step in your fertility journey.
For example, someone trying to conceive naturally may use fertility preparation to understand ovulation and improve timing.
Someone preparing for IVF may use it to support whole-body health before egg retrieval or embryo transfer. Someone considering egg freezing may use it to prepare for stimulation, retrieval, and the emotional weight of preserving future options.
Why Is Fertility Preparation Important?
Fertility preparation matters because reproductive health is connected to whole-body health.
For many people, the challenge is not only “How do I get pregnant?”
The deeper question is: “How do I prepare my body to support a healthy pregnancy and baby?”
Health Youniversity’s Preconception Plan states that this is not just about getting pregnant. It is about preparing the body to receive and nurture new life in the healthiest, most sustainable way possible.
That matters across every fertility path.
If you are trying naturally, fertility preparation can help you understand ovulation, fertile timing, sperm health, and when to seek support.
If you are navigating infertility, fertility preparation can help you gather the right medical information without blaming yourself or waiting too long.
If you are preparing for IVF, fertility preparation can help you support the body entering stimulation, retrieval, embryo development, transfer, and the two-week wait.
If you are freezing eggs, fertility preparation can help you understand your ovarian reserve, your timeline, your options, and the limits of what egg freezing can and cannot promise.
If you are preparing for pregnancy, fertility preparation helps you begin before a positive test, when many early developmental processes are already underway.
The CDC recommends planning before pregnancy by speaking with a healthcare provider, taking folic acid, stopping alcohol, smoking, and certain drugs, and avoiding toxic substances that can affect reproductive health.
Here’s what matters.
Fertility preparation is not about doing more. It is about doing what is most relevant, most supportive, and most aligned with your next step.
How Does Fertility Preparation Work?
Fertility preparation works by supporting the systems involved in conception, implantation, fertility treatment, and early pregnancy.
Area of Preparation
Why It Matters
Example
Medical readiness
Identifies conditions that may affect fertility or pregnancy
Preconception visit, medication review, thyroid or metabolic testing
Cycle awareness
Helps identify ovulation and timing
Tracking cycle length, cervical mucus, ovulation tests
Sperm health
Supports fertilization and embryo development
Semen analysis, lifestyle review, heat/toxin reduction
Egg and ovarian health
Supports fertility planning and treatment strategy
AMH, FSH, estradiol, antral follicle count when indicated
Uterine and tubal health
Supports implantation and natural conception pathways
Ultrasound, HSG, saline sonogram when clinically needed
Nutrition
Supports hormones, blood sugar, inflammation, and energy
Protein, healthy fats, fiber, colorful plants, hydration
Circulation
Supports reproductive organ nourishment
Gentle movement, qigong, acupoint stimulation, walking
Lifestyle
Reduces avoidable reproductive barriers
Sleep, toxin reduction, smoking cessation, alcohol reduction
Emotional support
Helps regulate stress and reduce isolation
Therapy, coaching, guided imagery, meditation, support systems
Think of fertility preparation as building the foundation before you build the house.
A healthy pregnancy begins before implantation. A strong IVF plan begins before stimulation. A thoughtful egg-freezing cycle begins before retrieval. A supported natural conception journey begins before the fertile window.
The Five Core Fertility Preparation Pathways
1. Infertility Preparation
Infertility preparation is about understanding why pregnancy has not happened yet and what information is needed next.
Infertility is commonly defined as not achieving pregnancy after 12 months or more of regular, unprotected intercourse. WHO defines infertility as a disease of the male or female reproductive system marked by failure to achieve pregnancy after 12 months or more of regular unprotected intercourse.
HealthYouniversity’s infertility guide emphasizes that infertility can involve female factors, male factors, both, or unexplained causes, and that evaluation should include ovulation, uterine and fallopian tube health, and semen analysis when sperm is part of the equation.
Infertility preparation may include:
Confirming how long you have been trying
Reviewing cycle regularity
Evaluating ovulation
Assessing sperm health
Reviewing uterine and tubal factors
Checking for PCOS, endometriosis, diminished ovarian reserve, thyroid concerns, or other relevant diagnoses
Creating an emotional support plan
ASRM recommends fertility evaluation after 12 months of trying for women under 35, after 6 months for women 35 or older, and more immediate evaluation for women over 40 or when a known fertility-related condition is present.
The better question is not, “Whose fault is this?”
The better question is, “Which part of the reproductive process needs more information or support?”
2. Natural Conception Preparation
Natural conception preparation is about supporting ovulation, timing, sperm health, and whole-body readiness without assisted reproductive treatment.
HealthYouniversity’s Natural Conception guide defines natural conception as pregnancy that happens without assisted reproductive treatments such as IUI, IVF, or ICSI. It also emphasizes that natural conception is not the same as “doing nothing.” It can still involve cycle tracking, preconception care, lab testing, nutrition, acupuncture, lifestyle changes, partner health support, and medical guidance.
The core pieces of natural conception preparation include:
Identifying the fertile window
Tracking cervical mucus or ovulation tests
Having intercourse regularly during the fertile window
Supporting sperm health
Taking folic acid or prenatal support
Reducing smoking, alcohol, recreational drugs, and high-impact toxic exposures
Seeking evaluation when the timeline or symptoms suggest it is time
ASRM defines the fertile window as the 6-day interval ending on the day of ovulation and notes that intercourse every 1–2 days during the fertile window can help maximize fecundability.
Many people think natural conception is only about timing sex.
The better way to understand it is this: natural conception depends on ovulation, sperm health, open reproductive pathways, implantation, nutrition, lifestyle, medical history, and whole-body health.
3. IVF Preparation
IVF preparation is about supporting the body before and during one of the most medically intensive fertility treatments.
IVF, or in vitro fertilization, is an assisted reproductive technology where eggs are retrieved from the ovaries, fertilized with sperm in a lab, and transferred as embryos into the uterus. Health Youniversity’s IVF guide highlights that IVF can be used for blocked fallopian tubes, ovulation disorders, endometriosis, male factor infertility, diminished ovarian reserve, genetic concerns, and unexplained infertility.
The CDC defines assisted reproductive technology as fertility treatments or procedures in which eggs or embryos are handled to help achieve pregnancy, and it identifies IVF as the most common type of ART.
IVF preparation may include:
Understanding why IVF is being recommended
Reviewing ovarian reserve and sperm testing
Preparing for stimulation medications
Creating a retrieval recovery plan
Asking about ICSI, PGT, fresh transfer, or frozen transfer
Supporting nutrition and hydration
Avoiding unapproved supplements
Planning emotional support before embryo updates and the two-week wait
IVF is not just a lab procedure.
It is a medical process that involves eggs, sperm, hormones, the uterine environment, embryo development, and the nervous system.
A strong IVF plan should include medical treatment and whole-body preparation.
4. Egg Freezing Preparation
Egg freezing preparation is about preserving future reproductive options while understanding the limits of the technology.
Egg freezing, also called oocyte cryopreservation, is a fertility preservation process where mature eggs are retrieved, frozen, and stored for possible future use. Health Youniversity’s Egg Freezing guide emphasizes that egg freezing can preserve options, but it does not guarantee a future pregnancy or live birth.
ASRM states that planned oocyte cryopreservation is ethically permissible and may help individuals avoid future infertility, while also emphasizing that people should be informed about uncertainties regarding effectiveness and long-term effects.
Egg freezing preparation may include:
Clarifying why you are freezing eggs
Reviewing age, AMH, antral follicle count, and expected egg yield
Asking how many mature eggs may be recommended for your goals
Understanding future thaw, fertilization, embryo development, and transfer steps
Preparing for medications, monitoring, retrieval, and recovery
Reviewing storage costs and consent decisions
Building emotional support before the cycle begins
Here’s the nuance.
Egg freezing can create possibilities. It cannot create certainty.
The goal is not to “pause fertility forever.” The goal is to preserve eggs at the age and health status they are when retrieved.
5. Pregnancy Readiness and Preconception Care
Pregnancy readiness is about preparing the body before conception so early pregnancy begins with more support.
HealthYouniversity’s pregnancy preparation guide defines pregnancy preparation as the process of supporting physical, reproductive, emotional, and lifestyle health before conception. It highlights medical care, folic acid, nutrition, movement, cycle awareness, toxin reduction, emotional support, and partner health.
ACOG recommends prepregnancy counseling that reviews medical, surgical, psychiatric, medication, supplement, family, genetic, immunization, nutrition, exercise, substance use, and environmental exposure history.
The CDC recommends that all women capable of becoming pregnant get 400 micrograms of folic acid daily to help prevent neural tube defects.
Pregnancy readiness may include:
Scheduling a preconception visit
Starting folic acid or prenatal support
Reviewing medications and supplements
Checking vaccines
Reviewing family and genetic history
Supporting nutrition and blood sugar balance
Reducing smoking, alcohol, recreational drugs, and harmful exposures
Supporting mental and emotional health
Including sperm health when relevant
Preparing for pregnancy is not just about the first positive test.
It is about building the foundation before conception begins.
Fertility Preparation by Pathway: Which Guide Should You Start With?

This is why a fertility preparation hub matters.
Each path is different, but the foundation overlaps: medical clarity, whole-body support, informed decisions, and emotional care.
The Health Youniversity Four-Pillar Fertility Preparation Framework
At the heart of Health Youniversity’s Preconception Plan are the Four Pillars of Fertility: Nutrition, Circulation, Lifestyle, and Emotional Support.
These four pillars should be used consistently across all five fertility content pillars because they give Health Youniversity a clear, recognizable fertility preparation method.
1. Nutrition
Nutrition supports hormone balance, egg health, sperm health, blood sugar, inflammation, energy, and early pregnancy development.
This does not mean following a perfect fertility diet.
It means giving the body consistent nourishment through:
Protein
Healthy fats
Fiber-rich carbohydrates
Colorful vegetables and fruits
Hydration
Prenatal nutrients when appropriate
Blood sugar-supportive meals
Provider-approved supplementation
Health Youniversity’s Preconception Plan includes cycle-specific nutrition guidance designed to support hormone balance and egg quality throughout the menstrual cycle.
2. Circulation
Circulation focuses on supporting blood flow to the ovaries, uterus, follicles, and reproductive tissues.
From a whole-health perspective, circulation may be supported through:
Walking
Gentle movement
Stretching
Qigong
Fertility yoga
Acupoint stimulation
Breathwork
Reducing sedentary patterns
Health Youniversity’s fertility model emphasizes targeted blood flow to the ovaries and uterus as part of reproductive organ support.
3. Lifestyle
Lifestyle includes the daily choices that shape reproductive health over time.
This may include:
Infertility preparation may include:
Sleep rhythm
Alcohol reduction
Smoking and vaping cessation
Caffeine moderation
Toxin reduction
Product swaps
Movement
Stress patterns
Medication and supplement review
Environmental exposure awareness
CDC guidance recommends avoiding harmful chemicals, environmental contaminants, and other toxic substances before pregnancy because these can affect reproductive systems.
The goal is not fear.
The goal is reducing the highest-impact avoidable exposures.
4. Emotional Support
Fertility is not only physical.
Trying to conceive, facing infertility, preparing for IVF, freezing eggs, or trying again after loss can bring grief, pressure, hope, fear, anger, and exhaustion.
Emotional support may include:
Therapy
Fertility coaching
Guided imagery
Meditation
Breathwork
Acupuncture or acupoint stimulation
Partner communication
Support groups
Boundaries around fertility conversations
HealthYouniversity’s program includes guided imagery, stress reduction, qigong, and individualized coaching to support the emotional side of fertility preparation.
This is not about “just relax.”
It is about helping your body and mind feel supported while you move through uncertainty.
When Should You Start Fertility Preparation?
The short answer: start as early as you can, but do not delay medical care to create a perfect plan.
For many people, a one-to-three-month preparation window is useful because it gives time to review medications, begin folic acid, improve nutrition, support sperm health, reduce toxic exposures, and understand the menstrual cycle.
The CDC notes that having enough folic acid in the body at least 1 month before and during pregnancy can help prevent major birth defects of the developing baby’s brain and spine.
HealthYouniversity’s Preconception Plan also notes that, from a TCM-informed perspective, a 3-month window can be helpful when possible because it gives the body time to restore balance, rebuild energy, and improve circulation for reproductive health.
But timing depends on your situation.
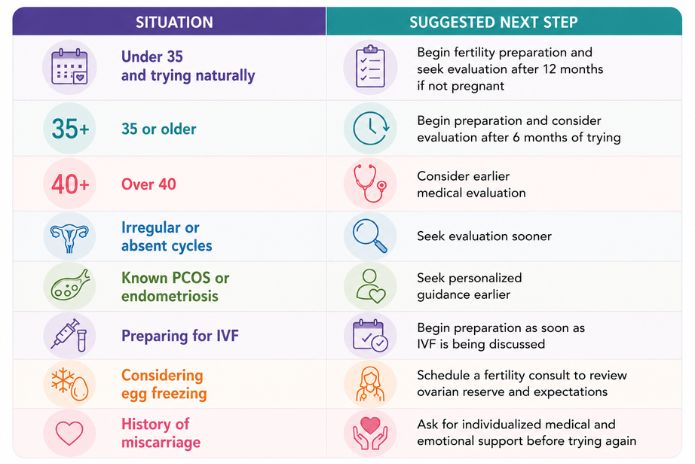
ASRM recommends fertility evaluation after 12 months of trying for women under 35, after 6 months for women 35 or older, and more immediate evaluation for women over 40 or when a known fertility-related condition is present.
The better question is not, “Whose fault is this?”
The better question is, “Which part of the reproductive process needs more information or support?”
What Should You Expect From Fertility Preparation?
Fertility preparation should feel clear, supportive, and individualized.
It should not feel like punishment, panic, or a list of impossible rules.
Here’s what to expect:
Expectation
What It Means
You may need medical testing
Testing depends on age, history, symptoms, and fertility goals
You may need partner testing
Sperm health matters for natural conception, IVF, and embryo development
You do not need a perfect diet
Consistency matters more than rigid restriction
You may need different support for different paths
IVF, egg freezing, natural conception, and pregnancy preparation each require specific planning
You may need emotional care
Fertility preparation includes the nervous system, not just the reproductive organs
You may need to act sooner
Age, diagnosis, recurrent loss, or irregular cycles can change the timeline
The better question is not, “Am I doing everything perfectly?”
The better question is, “Do I have a clear plan that supports my body, my fertility path, and my next decision?”
How to Start Fertility Preparation: Step-by-Step
Step 1: Identify Your Fertility Path
Start by naming where you are right now.
Are you:
Trying to conceive naturally?
Recently diagnosed with infertility?
Preparing for IVF?
Considering egg freezing?
Preparing for pregnancy after loss?
Trying to improve pregnancy readiness before actively trying?
This matters because each path has different timelines, tests, and decisions.
For example, someone preparing for egg freezing may need ovarian reserve testing and retrieval planning. Someone trying naturally may need fertile window education and sperm health support. Someone preparing for IVF may need medication planning, retrieval support, and embryo transfer preparation.
Step 2: Schedule a Preconception or Fertility Visit
A preconception visit is useful even if you are not yet infertile.
Use this visit to review:
Medical history
Menstrual cycle patterns
Prior pregnancies or losses
Medications
Supplements and herbs
Vaccines
Family history
Genetic risks
Partner health
Lifestyle exposures
Mental health
Fertility timeline
ACOG recommends prepregnancy counseling that reviews medical history, medications, supplements, genetic risks, immunizations, nutrition, exercise, substance use, and environmental exposures.
This visit helps turn vague concern into a practical plan.
Step 3: Start Folic Acid or Prenatal Support
Folic acid is one of the clearest evidence-based preconception steps.
CDC recommends 400 micrograms of folic acid daily for all women capable of becoming pregnant.
Ask your provider whether you need a prenatal vitamin or additional nutrients based on:
Vegan or vegetarian diet
Anemia history
Thyroid concerns
Vitamin D deficiency
Digestive disorders
Bariatric surgery
Prior neural tube defect pregnancy
Seizure medication use
Recurrent pregnancy loss
IVF or fertility treatment plan
Do not assume more supplements are always better.
The safest plan is personalized.
Step 4: Learn Your Cycle and Ovulation Pattern
Your menstrual cycle is one of the most useful windows into reproductive health.
Track for one to three months:
First day of bleeding
Cycle length
Cervical mucus
Ovulation predictor kit results
PMS symptoms
Spotting
Pain
Flow changes
Basal body temperature, if helpful
Intercourse timing
ASRM notes that fertility-awareness methods such as ovulation detection kits and cervical mucus monitoring can increase the probability of conceiving in a given menstrual cycle.
This helps you understand whether you may be ovulating and whether your fertile window is being identified accurately.
Step 5: Include Sperm Health From the Beginning
Fertility preparation is not only about the person carrying the pregnancy.
Sperm health matters for fertilization, embryo development, natural conception, IUI, and IVF.
Supportive steps may include:
Semen analysis when indicated
Stop smoking or vaping
Avoid recreational drugs
Reduce heavy alcohol use
Improve sleep
Eat antioxidant-rich foods
Avoid frequent hot tubs or sauna exposure
Review medications with a clinician
Address chronic health concerns
ASRM states that when a male partner is contributing to pregnancy, evaluation of both partners should begin at the same time, and at least one semen analysis should be obtained at the onset of infertility evaluation.
This is where many couples lose time.
Do not wait until every female-factor test is complete before asking about sperm.
Step 6: Build a Whole-Body Nutrition Foundation
Start with nourishment, not restriction.
A fertility-supportive plate may include:

Nutrition supports general health, but it should not be framed as a guarantee.
ASRM notes that a healthy lifestyle and diet should be encouraged in people attempting pregnancy for their effects on general health, while also noting insufficient evidence that one specific diet or macronutrient pattern improves natural fertility for everyone.
The goal is steady support.
Step 7: Reduce High-Impact Lifestyle Barriers
Start with the biggest barriers first.
Focus on:
Smoking
Vaping
Recreational drugs
Heavy alcohol use
High caffeine intake
Poor sleep
Unmanaged chronic conditions
Significant toxin exposure
Unreviewed medications or supplements
High stress without support
CDC recommends stopping alcohol, smoking, and certain drugs before pregnancy and avoiding toxic substances and contaminants that may affect reproductive health.
Small changes done consistently are usually more helpful than an extreme plan you cannot sustain.
Step 8: Support Circulation and Movement
Movement supports circulation, metabolic health, stress regulation, and connection to the body.
Helpful options may include:
Walking
Gentle stretching
Qigong
Fertility yoga
Light strength training
Breath-led movement
Acupoint stimulation, when appropriate
If you are in an active IVF or egg-freezing stimulation cycle, follow your clinic’s exercise restrictions. Enlarged ovaries may increase discomfort or risk with high-impact exercise, twisting, or intense abdominal movement.
The point is not to force intensity.
The point is to support blood flow, steadiness, and reproductive organ nourishment.
Step 9: Prepare Emotionally Before the Hardest Moments
Fertility preparation should include emotional planning before the most stressful moments arrive.
Ask yourself:
Who will know we are trying?
Who will know about IVF, egg freezing, or pregnancy testing?
What boundaries do I need?
How will I handle embryo updates?
What support do I need during the two-week wait?
What helps my nervous system feel safe?
What will I do if the result is not what I hoped for?
HealthYouniversity’s Preconception Plan includes guided imagery, stress reduction, qigong, and individualized coaching because fertility is more than physical.
This is not mindset pressure.
This is care.
Step 10: Know When to Ask for More Help
Fertility preparation should never become a reason to delay care when care is needed.
Seek medical guidance sooner if you have:
Irregular or absent periods
Known or suspected PCOS
Known or suspected endometriosis
Recurrent miscarriage
Prior ectopic pregnancy
Pelvic pain
History of pelvic infection
Known sperm concerns
Age over 40
Prior chemotherapy or radiation
Known uterine, tubal, or ovarian concerns
Difficulty conceiving after the recommended timeline
Seeking help does not mean you failed.
It means you are protecting your time, health, and options.
Fertility Preparation Checklist
Use this as a practical starting point.
Step
Natural Conception
IVF
Egg Freezing
Pregnancy Readiness
Preconception visit
Yes
Yes
Yes
Yes
Folic acid/prenatal support
Yes
Often yes
Ask provider
Yes
Cycle tracking
Yes
Helpful before cycle
Helpful context
Yes
Semen analysis
If delayed conception
Yes when sperm involved
If embryos may be created later
If sperm involved
Ovarian reserve testing
If indicated
Yes
Yes
If indicated
Uterine/tubal evaluation
If indicated
Often yes
Not always
If indicated
Medication review
Yes
Yes
Yes
Yes
Nutrition support
Yes
Yes
Yes
Yes
Toxin reduction
Yes
Yes
Yes
Yes
Emotional support
Yes
Yes
Yes
Yes
Common Mistakes to Avoid With Fertility Preparation
1. Waiting Until You Are Pregnant to Prepare
Many people begin thinking about pregnancy health after a positive test.
The problem is that early fetal development begins before many people know they are pregnant.
Better approach: Begin with a preconception visit, folic acid, medication review, and foundational health support before conception whenever possible.
2. Treating Fertility Preparation Like a Guarantee
Fertility preparation can support health, but it cannot guarantee pregnancy, IVF success, egg-freezing success, or live birth.
The problem is that early fetal development begins before many people know they are pregnant.
Better approach: Begin with a preconception visit, folic acid, medication review, and foundational health support before conception whenever possible.
3. Focusing Only on Egg Health
Egg health matters, but fertility also involves sperm, ovulation, tubes, uterus, hormones, metabolic health, immune factors, lifestyle, and age.
Better approach: Look at the whole reproductive process.
4. Ignoring Sperm Health
Sperm health is often evaluated too late.
Better approach: If sperm is part of the equation, include semen analysis and sperm-supportive lifestyle changes early, especially if conception is delayed.
5. Relying Only on an App to Predict Ovulation
Apps estimate based on past cycles. They do not confirm what your body is doing this month.
Better approach: Use cervical mucus, ovulation predictor kits, cycle patterns, and medical guidance when needed.
6. Taking Too Many Supplements Without Guidance
More supplements do not always mean better fertility.
Some supplements may interact with medications, affect bleeding risk, or be inappropriate during IVF, egg freezing, pregnancy, or certain diagnoses.
Better approach: Review supplements with your healthcare provider.
7. Doing an Extreme Detox
Aggressive detoxes, fasting, laxatives, or restrictive cleanses can stress the body.
Better approach: Focus on gentle, nourishing toxin reduction through food quality, hydration, sleep, product swaps, and regular elimination.
8. Waiting Too Long to Seek Fertility Evaluation
Some people keep trying naturally for years because they want to avoid medical intervention.
Better approach: Use age, cycle history, and risk factors to decide when to seek care. ASRM recommends evaluation after 12 months if under 35, after 6 months if 35 or older, and sooner when indicated.
Tools and Resources That Can Support Fertility Preparation
Fertility Assessment Quiz
A fertility quiz can help you identify whether your next step is natural conception support, infertility evaluation, IVF preparation, egg freezing preparation, or pregnancy readiness. Health Youniversity invites visitors to begin with a Fertility Assessment Quiz or a free assessment call.
Preconception Visit Checklist
Use this to organize medications, supplements, cycle history, family history, vaccines, prior pregnancies, losses, and fertility questions.
Cycle Tracking Journal
Track bleeding, cycle length, cervical mucus, ovulation tests, mood, sleep, pain, spotting, and intercourse timing.
Lab and Results Tracker
Track AMH, FSH, estradiol, progesterone, TSH, vitamin D, ferritin, semen analysis, HSG, SHG, ultrasound, and genetic screening when relevant.
IVF or Egg Freezing Question List
Use this to ask about protocol, medication side effects, retrieval expectations, embryo development, egg maturity, storage, costs, and future use.
Emotional Support Plan
Decide who supports you, what boundaries you need, and what practices help you stay grounded.
Health Youniversity Preconception Plan
HealthYouniversity’s Preconception Plan includes a 4-week self-paced protocol, acupoint stimulation, guided imagery meditations, qigong practices, recipes, sample menus, shopping lists, and individualized support for people preparing for natural conception, IVF, or egg freezing.
FAQs About Fertility Preparation
What is fertility preparation?
A fertility quiz can help you identify whether your next step is natural conception support, infertility evaluation, IVF preparation, egg freezing preparation, or pregnancy readiness. Health Youniversity invites visitors to begin with a Fertility Assessment Quiz or a free assessment call.
When should I start preparing for fertility?
Start as early as you can, ideally one to three months before trying to conceive or beginning fertility treatment. However, do not delay medical care to complete a perfect preparation plan, especially if you are over 35, have irregular cycles, have recurrent losses, or have a known fertility-related condition.
Can fertility preparation help with IVF?
Yes, fertility preparation can support the body before and during IVF by improving medical readiness, nutrition, hydration, lifestyle routines, emotional support, and communication with your fertility team. It does not guarantee IVF success, but it can help you enter treatment with more clarity and support.
Can fertility preparation help with egg freezing?
Yes. Fertility preparation can help you understand ovarian reserve, prepare for stimulation and retrieval, support whole-body health, and ask better questions about egg maturity, storage, future use, and realistic expectations. Egg freezing can preserve future options, but it does not guarantee a future pregnancy or live birth.
What should I do first if I am trying to conceive naturally?
Start with cycle awareness, folic acid or prenatal support, regular intercourse during the fertile window, sperm health support, and a preconception visit. ASRM notes that the fertile window is the 6-day interval ending on ovulation day and that intercourse every 1–2 days during that window can help maximize fecundability.
When should I see a fertility specialist?
Consider evaluation after 12 months of trying if the female partner is under 35, after 6 months if she is 35 or older, and sooner if she is over 40 or has irregular cycles, recurrent miscarriage, PCOS, endometriosis, pelvic pain, known sperm concerns, or other fertility-related risk factors.
Is fertility preparation only for women?
No. Fertility preparation includes sperm health when sperm is part of the plan. Sperm health can affect fertilization and embryo development, so male partner evaluation and lifestyle support may be important.
What vitamins should I take before pregnancy?
Folic acid is the most important starting point for most people who can become pregnant. CDC recommends 400 micrograms of folic acid daily for all women capable of becoming pregnant. Ask your provider whether you also need prenatal vitamins, iron, vitamin D, iodine, B12, omega-3s, choline, or other nutrients.
Does fertility preparation guarantee pregnancy?
No. Fertility preparation does not guarantee pregnancy, IVF success, egg-freezing success, or live birth. It supports the body, improves readiness, helps reduce avoidable barriers, and helps you make more informed decisions.
What is the HealthYouniversity approach to fertility preparation?
Health Youniversity uses a whole-health approach that blends Traditional Chinese Medicine, Functional Medicine, fertility education, and practical self-care tools. Its Preconception Plan centers on four pillars: Nutrition, Circulation, Lifestyle, and Emotional Support.
Conclusion
Fertility preparation is not just about getting pregnant.
It is about understanding your body, supporting your reproductive health, preparing emotionally, and making informed decisions before natural conception, IVF, egg freezing, or pregnancy.
The path may look different depending on where you are. Natural conception may begin with cycle awareness and timing. Infertility may require evaluation and testing. IVF may require stimulation, retrieval, embryo development, and transfer planning. Egg freezing may require ovarian reserve testing and realistic expectations. Pregnancy readiness may begin with folic acid, medical review, and whole-body support.
But the foundation is the same: your reproductive health is connected to your whole health.
If you are preparing for natural conception, IVF, egg freezing, or pregnancy after infertility or loss, Health Youniversity’s Preconception Plan can help you build a clearer, more supported fertility foundation with nutrition, circulation, lifestyle guidance, and emotional care.

About The Author
Dr. Susan Fox
DACM, L.Ac., FABORM
Fertility Coach/Expert, Founder of Health Youniversity
Dr. Susan Fox, DACM, L.Ac., FABORM, is a fertility coach, Doctor of Acupuncture and Chinese Medicine, and Founder of Health Youniversity. She has 24 years of experience supporting women ages 30–45 navigating natural conception, IVF, IUI, PCOS, endometriosis, diminished ovarian reserve, and unexplained infertility. Her work blends Traditional Chinese Medicine, Functional Medicine, fertility education, nutrition, circulation support, lifestyle medicine, and emotional well-being to help women prepare their bodies for conception and pregnancy.
Follow the expert:
© 2026 Your Fertile Health LLC. All rights reserved. The content of this website, including but not limited to text, graphics, images, and any other material contained on this website,
is for informational purposes only and is the property of Your Fertile Health LLC. Unauthorized use, distribution, or reproduction is strictly prohibited.


