Natural Conception: How It Works, When to Try, and How to Support Fertility Naturally
Written by: Dr. Susan Fox, DACM, L.Ac., FABORM
Credentials: Fertility and Women’s Health Expert, Founder of HealthYouniversity
Updated: May 2026
Medical disclaimer: This article is educational and does not replace medical advice from your physician, OB-GYN, reproductive endocrinologist, urologist, midwife, oncologist, or licensed healthcare provider.
Key Takeaways
Natural conception means becoming pregnant without assisted reproductive treatments such as IUI, IVF, or ICSI.
Natural conception is not the same as “doing nothing.” It can still involve cycle tracking, preconception care, sperm health support, lab testing, lifestyle changes, nutrition, acupuncture, and medical guidance.
The fertile window is the most important timing factor. ASRM defines it as the 6-day interval ending on the day of ovulation.
Intercourse every 1–2 days during the fertile window can help maximize fecundability, while intercourse 2–3 times per week throughout the cycle is also a practical approach for many couples.
Natural conception depends on ovulation, sperm health, reproductive anatomy, timing, nutrition, lifestyle, medical history, and whole-body health.
If pregnancy has not happened after 12 months of trying, or after 6 months if the female partner is 35 or older, fertility evaluation is recommended. Earlier evaluation may be needed with irregular cycles, known fertility conditions, recurrent miscarriage, or age over 40.
Quick Answer
Natural conception is pregnancy that happens without assisted reproductive treatments such as IUI, IVF, or ICSI. It occurs when ovulation happens, sperm reaches and fertilizes the egg, the fertilized egg develops, and the embryo implants in the uterus. To support natural conception, focus on identifying the fertile window, timing intercourse, supporting sperm health, taking folic acid or prenatal support, improving whole-body health, and knowing when to seek fertility evaluation.
Introduction
Natural conception can sound simple: track ovulation, have sex at the right time, and wait for a positive pregnancy test.
But for many people, trying to conceive naturally becomes confusing quickly. Apps give different predictions. Ovulation tests are not always clear. Cycles shift. Stress builds. And after a few months, it can be hard to know whether you need more patience, better timing, or professional support.
Here’s what matters: natural conception is not only about timing sex.
It is about understanding ovulation, protecting sperm health, preparing the body before pregnancy, reducing avoidable barriers, and knowing when medical support is the next right step.
In this guide, you’ll learn what natural conception means, how it works, how to identify the fertile window, what lifestyle factors matter, what mistakes to avoid, and when to seek fertility care.

What Is Natural Conception?
Natural conception is pregnancy that happens without assisted reproductive treatments such as intrauterine insemination, in vitro fertilization, or intracytoplasmic sperm injection.
In practical terms, natural conception happens when:
Ovulation occurs.
Sperm reaches the egg.
Fertilization takes place.
The fertilized egg develops.
The embryo implants in the uterus.
Natural conception is not the same as “doing nothing.”
It can still include cycle tracking, preconception care, lab testing, lifestyle changes, partner health support, acupuncture, nutrition planning, and medical guidance.
For example, a couple trying to conceive naturally may track cervical mucus, use ovulation predictor kits, take folic acid, improve nutrition, review medications, reduce toxic exposures, and seek testing if pregnancy does not happen within the expected timeframe.
What Natural Conception Is Not
Natural Conception: What It Is, How It Works, and How to Support It
Natural conception is not:
A guarantee that pregnancy will happen quickly
A reason to avoid medical care
Only about the female partner
Only about having sex on ovulation day
A sign that you should never use fertility support
The same as waiting indefinitely
A replacement for evaluation when there are symptoms or risk factors
Many people think natural conception means “just keep trying.”
The better way to understand it is this: natural conception works best when you understand your cycle, time intercourse appropriately, support sperm health, prepare the body before pregnancy, and ask for help when your history suggests you should not wait.
Why Is Natural Conception Important?
Natural conception matters because it is often the first path people try when they want to grow their family.
It also gives useful information about reproductive health. Your menstrual cycle, ovulation signs, fertile window, sperm health, and time to pregnancy can all reveal whether your body may need more support.
The CDC explains that health before pregnancy can affect the health of a future baby and recommends planning ahead by talking with a healthcare provider, taking folic acid, stopping alcohol, smoking, and certain drugs, and avoiding toxic substances that may affect reproductive health.
For many people, the deeper challenge is not a lack of effort.
It is a lack of clear, trustworthy information.
That is where a structured natural conception plan can help.
How Does Natural Conception Work?
Natural conception works through a sequence of reproductive events.
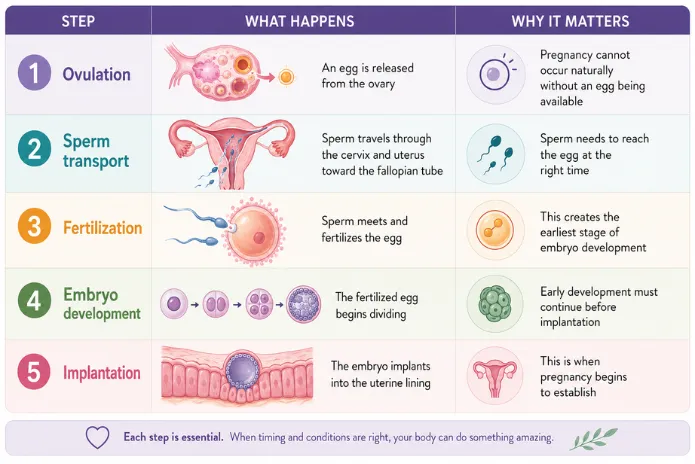
Timing matters because the egg and sperm have different survival windows.
Sperm can survive in the reproductive tract for several days. The egg survives for a much shorter time after ovulation. That is why the fertile window includes the days before ovulation, not only the day ovulation happens.
ASRM defines the fertile window as the 6-day interval ending on the day of ovulation. It also notes that peak fecundability has been observed when intercourse occurs within the two days before ovulation.
What Is the Fertile Window?
The fertile window is the group of days in the menstrual cycle when pregnancy is most likely to occur.
For most people, this includes the five days before ovulation and the day of ovulation.
The biggest misconception is that you only need to have sex on ovulation day. In reality, the days before ovulation are often the most important because sperm needs to be present when the egg is released.
Timing Strategy
Best For
Why It Helps
Intercourse every 1–2 days during the fertile window
People actively tracking ovulation
Keeps sperm available during the highest-fertility days
Intercourse 2–3 times per week throughout the cycle
People who do not want to track closely
Reduces the chance of missing ovulation
Cervical mucus + ovulation tests
People with variable cycles
Uses current-cycle signs instead of relying only on a calendar
Calendar app alone
Basic cycle logging
Helpful for recording data, but less reliable for precise ovulation timing
ASRM notes that fertility-awareness methods, such as ovulation detection kits and cervical mucus monitoring, can increase the probability of conceiving in a given menstrual cycle. It also notes that the fertile window can vary even in people with regular cycles.
Natural Conception vs. IUI vs. IVF
Option
How It Works
Best For
Main Limitation
Natural conception
Sperm and egg meet inside the body
People with regular ovulation, open tubes, and adequate sperm health
Timing, sperm, ovulation, tubal, or uterine factors may interfere
IUI
Prepared sperm is placed into the uterus around ovulation
Mild male factor, donor sperm, unexplained infertility, timing concerns
Fertilization still happens inside the body
IVF
Eggs are retrieved and fertilized in a lab, then embryos are transferred
Tubal disease, significant male factor, endometriosis, genetic testing needs, failed prior treatments
More medically intensive, costly, and emotionally demanding
Natural conception is not “better” or “worse” than fertility treatment.
It is one path. The right path depends on your age, cycle pattern, sperm health, fallopian tube status, medical history, timeline, and goals.
The Main Pillars of Natural Conception
1. Ovulation and Cycle Health
Ovulation is central to natural conception.
If you are not ovulating, or if ovulation is irregular, timing intercourse becomes much harder. Regular cycles can be a helpful sign, but they do not always guarantee that ovulation is happening every cycle.
Common signs of ovulation may include:
Slippery or stretchy cervical mucus
A positive ovulation predictor kit
Mild pelvic sensation or ovulation pain
A shift in basal body temperature after ovulation
More predictable cycle patterns
If cycles are consistently shorter than 21 days, longer than 35 days, absent, or highly irregular, it is worth speaking with a healthcare provider.
2. Fertile Window Timing
Timing intercourse during the fertile window increases the chance that sperm is present when ovulation occurs.
ASRM states that reproductive efficiency is highest when intercourse occurs every 1–2 days during the fertile window, but also notes that results from intercourse 2–3 times per week are nearly equivalent for many couples.
The goal is not to hit one perfect day.
The goal is to avoid missing the fertile window.
3. Sperm Health
Natural conception depends on sperm health as much as egg and ovulation health.
Semen quality can be affected by:
Smoking
Marijuana or recreational drug use
Alcohol
Heat exposure
Some medications
Chronic illness
Sleep
Weight
Environmental exposures
Medical conditions
ASRM recommends semen evaluation when applicable as part of fertility evaluation, and parallel evaluation of the male partner should occur when relevant.
This is important because many couples spend months focusing only on the female partner’s cycle, even though male factors can also contribute to difficulty conceiving.
4. Preconception Nutrition
Nutrition supports the body before conception.
There is no single “perfect fertility diet” that guarantees pregnancy. But consistent nourishment can support hormone balance, blood sugar, inflammation, egg health, sperm health, and early pregnancy development.
Focus on:
Protein at meals
Vegetables and fruits
Healthy fats
Beans and legumes
Fiber-rich carbohydrates
Low-mercury seafood
Nuts and seeds
Hydration
A prenatal vitamin or folic acid, when appropriate
CDC recommends that all women capable of becoming pregnant get 400 micrograms of folic acid daily to help prevent neural tube defects.
5. Lifestyle and Environmental Support
Lifestyle does not control every fertility outcome, but it can reduce avoidable barriers.
The CDC recommends stopping alcohol, smoking, and certain drugs before pregnancy and avoiding harmful chemicals, environmental contaminants, and toxic substances at home and work.
ASRM also notes that alcohol abuse, recreational drugs, smoking, and high caffeine intake may negatively affect fertility.
Practical changes may include:
Stop smoking or vaping.
Avoid recreational drugs.
Reduce or avoid alcohol while trying to conceive.
Keep caffeine moderate.
Avoid heating food in plastic.
Choose fragrance-free or lower-toxin products when possible.
Wash produce well.
Review workplace exposures if relevant.
The goal is not fear.
The goal is reducing the biggest avoidable exposures.
6. Emotional and Nervous System Support
Trying to conceive naturally can be emotionally intense.
Even when everything looks “normal,” the waiting can create stress, pressure, disappointment, and self-blame.
Health Youniversity’s whole-health model includes emotional support as one of the pillars of fertility preparation, with tools to reduce stress, reconnect with the body, and feel supported through the process.
Emotional support may include:
Therapy
Fertility coaching
Breathwork
Guided imagery
Meditation
Acupuncture or acupoint stimulation
Journaling
Partner communication
Support groups
Stress support is not about forcing yourself to “just relax.”
It is about helping your body and mind feel safer while you move through uncertainty.
The Health Youniversity Four-Pillar Natural Conception Framework
Health Youniversity’s fertility model should be consistently used across the website as the Four Pillars of Fertility: Nutrition, Circulation, Lifestyle, and Emotional Support. The audit specifically recommends using this method on the Natural Conception page to show how the four pillars support ovulation, sperm health, and implantation.
1. Nutrition
Nutrition supports hormone balance, blood sugar, inflammation, egg health, sperm health, and early pregnancy development.
A practical example: Build meals around protein, healthy fats, fiber-rich carbohydrates, colorful plants, and hydration.
2. Circulation
Circulation focuses on blood flow and reproductive organ support.
A practical example: Walking, gentle movement, stretching, qigong, acupuncture, or acupoint stimulation may help support the body before conception.
3. Lifestyle
Lifestyle includes sleep, toxin reduction, alcohol and tobacco avoidance, caffeine moderation, movement, and daily routines.
A practical example: Stop smoking, reduce alcohol, avoid heating food in plastic, and review medications or supplements with your provider.
4. Emotional Support
Emotional support helps reduce isolation and supports the nervous system while trying to conceive.
A practical example: Use guided imagery, therapy, fertility coaching, meditation, breathwork, or a support group instead of carrying the process alone.
How Long Does Natural Conception Take?
The short answer: it depends.
Time to conception can vary based on age, ovulation, sperm health, intercourse frequency, medical history, cycle regularity, reproductive anatomy, and overall health.
Many healthy couples do not conceive in the first month of trying. That does not always mean something is wrong.
However, timing matters.
ASRM recommends infertility evaluation after 12 months of trying for women under 35, after 6 months for women 35 or older, and more immediate evaluation for women over 40 or when there is a known medical history associated with infertility.
Situation
Under 35 with regular cycles and no known risk factors
Age 35 or older
Over 40
Irregular or absent periods
Known or suspected PCOS
Known or suspected endometriosis
Recurrent miscarriage
Previous ectopic pregnancy
Known sperm concerns
Pelvic pain or painful periods
Prior chemotherapy, radiation, or ovarian surgery
When to Seek Fertility Support
After 12 months of trying
After 6 months of trying
Consider more immediate evaluation
Seek care sooner
Seek care sooner
Seek care sooner
Seek care sooner
Seek care sooner
Seek care sooner
Seek care sooner
Seek care sooner
The most important thing is not to wait too long when your history suggests you need support.
Natural Conception Tracking Methods: Which Ones Help?
Method
What It Does
Best For
Limitation
Calendar app
Estimates fertile days based on past cycles
Basic cycle logging
Less accurate if cycles vary
Cervical mucus tracking
Uses body signs to identify fertile days
Current-cycle awareness
Takes practice
Ovulation predictor kits
Detects LH surge before ovulation
Timing intercourse
Can be confusing with PCOS or irregular LH patterns
Basal body temperature
Confirms ovulation after it happens
Pattern recognition
Not ideal for predicting fertile days in advance
Cycle symptom journal
Tracks PMS, pain, spotting, and patterns
Understanding cycle health
Not a standalone fertility tool
Semen analysis
Evaluates sperm count, motility, and morphology
Delayed conception or male risk factors
Requires lab testing
The best method depends on your cycle, stress level, intercourse frequency, and how much tracking feels helpful versus overwhelming.
How to Support Natural Conception: Step-by-Step
Step 1: Schedule a Preconception Visit
Start with a preconception visit with your OB-GYN, primary care provider, midwife, or fertility specialist.
Use this visit to review:
Medical history
Current diagnoses
Medications
Supplements
Vaccines
Menstrual cycle patterns
Prior pregnancies or losses
Family history
Lifestyle factors
Mental health
Partner health
CDC recommends talking with a healthcare provider before pregnancy about health history, current medical conditions, medications, vaccinations, lifestyle, and behavior.
Practical tip: Bring a list of your medications, supplements, cycle patterns, and how long you have been trying.
Step 2: Start Folic Acid or a Prenatal Vitamin
Start folic acid before pregnancy.
CDC recommends 400 micrograms of folic acid daily for all women capable of becoming pregnant. This matters because neural tube defects can happen very early in pregnancy, often before someone knows they are pregnant.
Ask your provider whether you need a prenatal vitamin, folic acid, methylfolate, iron, vitamin D, iodine, B12, omega-3, choline, or other support based on your health history and labs.
Practical tip: Do not add a long list of supplements without professional guidance.
Step 3: Learn Your Cycle
Begin tracking your cycle for at least one to three months.
Track:
First day of bleeding
Cycle length
Cervical mucus
Ovulation test results
PMS symptoms
Spotting
Pain
Sleep and stress patterns
Intercourse timing
This helps you see whether your cycle is predictable and whether you may be identifying your fertile window accurately.
Practical tip: Do not rely on an app alone if your cycles vary.
Step 4: Identify the Fertile Window
Use current-cycle signs instead of relying only on a calendar app.
Helpful signs may include:
Slippery, stretchy cervical mucus
A positive LH ovulation test
A predictable pattern of ovulation symptoms
Basal body temperature shift after ovulation
Cervical mucus and ovulation predictor kits are often more useful than calendar counting alone because they reflect what your body is doing in the current cycle.
Practical tip: The days before ovulation matter. Do not wait until ovulation day to start trying.
Step 5: Time Intercourse Without Overcomplicating It
The goal is to have sperm available before ovulation.
ASRM states that reproductive efficiency is highest when intercourse occurs every 1–2 days during the fertile window, but intercourse 2–3 times per week gives nearly equivalent results for many couples.
A simple plan:
If you track ovulation: have intercourse every 1–2 days during the fertile window.
If you do not track: have intercourse 2–3 times per week throughout the cycle.
If timing is stressful: choose consistency over perfection.
Practical tip: Do not turn timing into pressure if it is harming intimacy or emotional health.
Step 6: Support Sperm Health
Include the sperm partner from the beginning.
Sperm-supportive steps may include:
Stop smoking or vaping.
Avoid marijuana and recreational drugs.
Reduce heavy alcohol use.
Improve sleep.
Eat antioxidant-rich foods.
Avoid frequent hot tub or sauna exposure.
Review medications with a clinician.
Consider semen analysis if conception is delayed.
Many people think natural conception means “just keep trying.”
The better way to understand it is this: natural conception works best when you understand your cycle, time intercourse appropriately, support sperm health, prepare the body before pregnancy, and ask for help when your history suggests you should not wait.
Step 7: Build a Fertility-Supportive Nutrition Pattern
Do not build your plan around restriction.
Build it around nourishment.
A simple fertility-supportive plate may include:
Protein
Healthy fats
Fiber-rich carbs
Colorful plants
Hydration
Eggs, fish, poultry, beans, lentils, tofu, Greek yogurt
Avocado, olive oil, nuts, seeds, low-mercury fish
Oats, quinoa, beans, lentils, sweet potatoes, fruit
Leafy greens, berries, herbs, cruciferous vegetables
Water, mineral-rich fluids, provider-approved herbal teas
ASRM encourages a healthy lifestyle and diet for people attempting pregnancy for their effects on general health, while noting there is insufficient evidence that one specific diet or macronutrient pattern improves natural fertility for everyone.
Practical tip: Focus on consistency, not perfection.
Step 8: Reduce High-Impact Fertility Barriers
Start with the biggest barriers first.
These include:
Smoking
Vaping
Marijuana
Recreational drugs
Heavy alcohol use
High caffeine intake
Poorly managed chronic conditions
Unreviewed medications
Significant toxin exposure
Untreated thyroid, metabolic, or reproductive concerns
ASRM notes that smoking, recreational drugs, alcohol abuse, and high caffeine intake may negatively affect fertility.
Practical tip: Choose the highest-impact change first instead of trying to overhaul everything at once.
Step 9: Review Vaccines and Family History
Before pregnancy, review your vaccine record and family health history.
ACOG recommends prepregnancy counseling that includes medical, surgical, psychiatric, medication, supplement, family, genetic, immunization, nutrition, exercise, substance use, and environmental exposure history.
Ask about:
MMR immunity
Varicella immunity
Flu vaccine
COVID-19 vaccine
Tdap timing
Hepatitis B, if relevant
Genetic carrier screening
Family history of birth defects, genetic conditions, recurrent miscarriage, or infant loss
Practical tip: Some vaccines are recommended before pregnancy, while others are given during pregnancy. Ask your provider what applies to you.
Step 10: Know When to Ask for Help
Natural conception does not mean avoiding medical support.
Ask for help if:
You are under 35 and have tried for 12 months without pregnancy.
You are 35 or older and have tried for 6 months.
You are over 40.
Your cycles are irregular or absent.
You have recurrent pregnancy loss.
You suspect endometriosis, PCOS, or male factor infertility.
You have pelvic pain, prior pelvic infection, or known tubal concerns.
Seeking support does not mean you failed.
It means you are protecting your time, your health, and your options.
Natural Conception Preparation Checklist
Natural Conception: What It Is, How It Works, and How to Support It
Natural conception is not:
Preparation Area
Preconception visit
Folic acid/prenatal support
Cycle tracking
Fertile window timing
Sperm health
Nutrition
Lifestyle
Emotional support
Medical evaluation
What to Do
Review medical history, medications, vaccines, and goals
Start provider-approved folic acid or prenatal support
Track cycle length, mucus, ovulation tests, pain, and bleeding
Have intercourse every 1–2 days during the fertile window or 2–3 times weekly
Include semen analysis when needed and support sperm lifestyle factors
Eat protein, healthy fats, fiber, colorful plants, and hydrate
Reduce smoking, alcohol, drugs, high caffeine, and toxic exposures
Build support before stress increases
Seek care based on age, timeline, and symptoms
Why It Matters
Helps identify issues before pregnancy
Supports early fetal development
Helps identify ovulation and patterns
Reduces chance of missing ovulation
Supports fertilization and embryo development
Supports whole-body fertility health
Reduces avoidable barriers
Helps reduce isolation and pressure
Protects time and fertility options
Common Mistakes to Avoid When Trying to Conceive Naturally
1. Relying Only on Day 14
Not everyone ovulates on day 14.
Ovulation timing can shift from cycle to cycle, even in people with regular periods.
Better approach: Track current-cycle signs such as cervical mucus and ovulation tests.
2. Having Sex Only Once During the Fertile Window
Trying to hit one perfect day can increase stress and reduce your chances of catching the fertile window.
Better approach: Have intercourse every 1–2 days during the fertile window or 2–3 times per week throughout the cycle.
3. Ignoring Sperm Health
Fertility is not only about the person ovulating.
Sperm health matters for fertilization and embryo development.
Better approach: Include partner lifestyle, medical history, and semen testing when appropriate.
4. Taking Too Many Supplements
More supplements do not always mean better fertility.
Some supplements may be unnecessary, low-quality, or inappropriate for your health history.
Better approach: Start with folic acid or a prenatal vitamin, then personalize based on labs and professional guidance.
5. Waiting Too Long to Seek Evaluation
Some people wait years before asking for help because they want to keep trying naturally.
Better approach: Use age, cycle history, and risk factors to decide when to seek care. ASRM recommends evaluation after 12 months if under 35, after 6 months if 35 or older, and sooner when indicated.
6. Treating Stress Like a Personal Failure
Stress is not a moral failure, and it is not helpful to tell someone to “just relax.”
Better approach: Build emotional support into the process through therapy, coaching, breathwork, guided imagery, or a support system.
7. Confusing Natural With Unsupported
Natural conception can still be guided, informed, and supported.
Better approach: Combine medical care, body literacy, lifestyle support, and whole-health fertility preparation.
8. Staying Supine After Sex Because You Think It Is Required
Many people believe they need to lie down for a long time after sex to help sperm travel.
ASRM notes that this belief has no scientific foundation and that sperm deposited at the cervix at midcycle can be found in the fallopian tubes within minutes.
Better approach: Do not add rituals that increase stress unless your clinician specifically recommends them.
What Tests Might Be Helpful Before or During Natural Conception?
The right testing depends on your age, cycle pattern, medical history, and how long you have been trying.
Possible tests to discuss with your provider include:
Test or Evaluation
CBC
Ferritin and iron
Thyroid panel
Vitamin D
A1c or fasting glucose
Rubella and varicella immunity
STI screening
Genetic carrier screening
Semen analysis
Progesterone testing
HSG or saline ultrasound
Why It May Matter
Screens for anemia or general health concerns
Helps assess iron stores
Thyroid function can affect cycles and pregnancy
May be useful if deficiency risk is present
Supports metabolic and blood sugar awareness
Helps identify vaccine needs before pregnancy
Supports reproductive and pregnancy health
Helps identify inherited condition risks
Evaluates sperm count, motility, and morphology
May help confirm ovulation in some cases
May evaluate fallopian tubes or uterine cavity if indicated
ASRM states that infertility evaluation should include ovulatory status, reproductive tract structure and patency, and semen evaluation of the male partner when applicable.
Tools and Resources to Support Natural Conception
Fertility Assessment Quiz
A quiz can help identify where you may need more support, especially if you are unsure whether your main challenge is timing, cycle health, stress, nutrition, or whole-body readiness.
Cycle Tracking Journal
Use this to track your period, cervical mucus, ovulation test results, mood, sleep, symptoms, and intercourse timing.
Ovulation Predictor Kits
These can help identify the LH surge before ovulation. They are often most helpful when used alongside cervical mucus and regular intercourse.
Preconception Visit Checklist
Bring your medication list, supplement list, cycle notes, family history, vaccination records, and questions.
Semen Analysis
If conception is delayed or there are sperm risk factors, semen analysis can provide useful information. ASRM recommends semen evaluation when applicable as part of fertility evaluation.
Whole-Health Fertility Program
Health Youniversity’s Preconception Plan supports people preparing for natural conception, IVF, or egg freezing with nutrition, circulation, lifestyle support, and emotional care.
FAQs
What is natural conception?
Natural conception is pregnancy that happens without assisted reproductive treatments such as IUI, IVF, or ICSI. It usually involves ovulation, sperm reaching the egg, fertilization, embryo development, and implantation.
How can I increase my chances of natural conception?
Focus on timing intercourse during the fertile window, taking folic acid, supporting sperm health, improving nutrition, reducing smoking and alcohol, and seeking medical guidance when appropriate. Intercourse every 1–2 days during the fertile window can help maximize fecundability.
When is the best time to have sex to get pregnant?
The best time is during the fertile window, especially the days leading up to ovulation. ASRM defines the fertile window as the 6-day interval ending on the day of ovulation.
Do I need to track ovulation to conceive naturally?
Not always. Many couples can try intercourse 2–3 times per week throughout the cycle. Tracking can be helpful if cycles are irregular, intercourse is less frequent, or you want a clearer understanding of your fertile window.
Are ovulation apps accurate?
Apps can be useful for logging cycle data, but calendar-only predictions may miss ovulation if your cycle varies. Current-cycle signs such as cervical mucus and ovulation predictor kits are often more useful.
How long should we try naturally before seeing a doctor?
ASRM recommends fertility evaluation after 12 months of trying if the female partner is under 35, after 6 months if she is 35 or older, and sooner if she is over 40 or has known fertility risk factors.
Does sperm health matter for natural conception?
Yes. Sperm health matters for fertilization and embryo development. If conception is delayed, semen analysis should be part of the evaluation when sperm is involved.
What should I avoid while trying to conceive naturally?
Avoid smoking, vaping, recreational drugs, and heavy alcohol use. Limit high caffeine intake and reduce avoidable toxic exposures where possible. CDC also recommends avoiding harmful chemicals and toxic substances at home and work before pregnancy.
Does lying down after sex improve chances of pregnancy?
There is no strong evidence that staying supine after intercourse improves natural conception. ASRM notes that postcoital routines such as remaining supine have no scientific foundation for improving sperm transport.
Can lifestyle changes guarantee natural conception?
No. Lifestyle changes cannot guarantee pregnancy. However, nutrition, folic acid, smoking cessation, reduced alcohol, sleep, movement, toxin reduction, and emotional support can support whole-body fertility and pregnancy readiness.
Conclusion
Natural conception is not just about timing sex.
It is about understanding your cycle, supporting ovulation, protecting sperm health, preparing your body before pregnancy, and knowing when to seek help. The goal is not to make the process perfect. The goal is to make it clearer, healthier, and less lonely.
If you are trying to conceive naturally, preparing for IVF, or wondering whether your body needs more support, Health Youniversity’s Preconception Plan can help you build a whole-body fertility foundation with nutrition, circulation, lifestyle support, and emotional care.
Take the Fertility Quiz, explore the Preconception Plan, or schedule a Fertility Assessment Call with Health Youniversity
Resources and Reference Links
ASRM: Optimizing Natural Fertility Committee Opinion — fertile window, intercourse timing, fertility-awareness methods, lifestyle factors, folic acid, and coital practices. https://www.asrm.org/practice-guidance/practice-committee-documents/optimizing-natural-fertility-a-committee-opinion-2021/
ASRM: Fertility Evaluation of Infertile Women Committee Opinion — when to seek evaluation, age-based timing, ovulation, reproductive tract assessment, and semen evaluation. https://integration.asrm.org/practice-guidance/practice-committee-documents/fertility-evaluation-of-infertile-women-a-committee-opinion-2021/
CDC: Planning for Pregnancy — preconception planning, folic acid, stopping alcohol/smoking/drugs, and avoiding toxic substances. https://www.cdc.gov/pregnancy/about/index.html
CDC: About Folic Acid — 400 mcg folic acid recommendation and neural tube defect prevention. https://www.cdc.gov/folic-acid/about/index.html
CDC: Folic Acid Sources and Recommended Intake — supplement and fortified-food guidance for reaching 400 mcg daily. https://www.cdc.gov/folic-acid/about/intake-and-sources.html
ACOG / Prepregnancy Counseling Guidance — use as a supporting resource for medication, vaccine, nutrition, exercise, substance use, and environmental exposure review. https://www.cdc.gov/pregnancy/about/index.html

About The Author
Dr. Susan Fox
DACM, L.Ac., FABORM
Fertility and Women’s Health Expert, Founder of Health Youniversity
Dr. Susan Fox has 24 years of experience in women’s health and fertility support, with expertise in fertility coaching, IVF preparation, natural conception, IUI, PCOS, endometriosis, diminished ovarian reserve, and unexplained infertility. She is a Licensed Acupuncturist in California, a Health and Wellness Coach, and a Fellow of the Acupuncture & TCM Board of Reproductive Medicine.
© 2026 Your Fertile Health LLC. All rights reserved. The content of this website, including but not limited to text, graphics, images, and any other material contained on this website,
is for informational purposes only and is the property of Your Fertile Health LLC. Unauthorized use, distribution, or reproduction is strictly prohibited.


